Treatment Plans
Generate detailed, professional medical treatment plans for clinical use
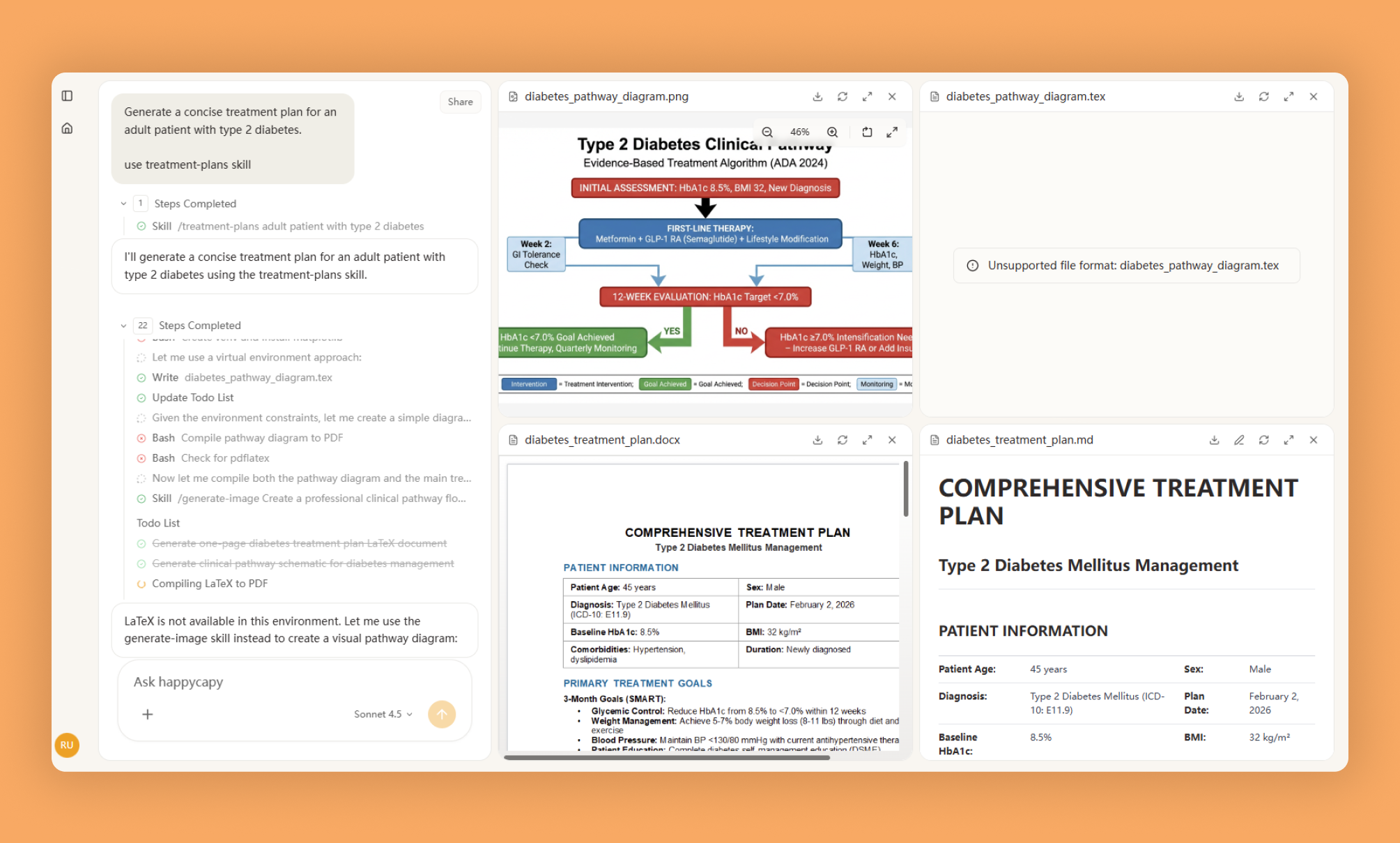
Healthcare providers need to create comprehensive treatment plans documenting diagnosis, interventions, goals, and follow-up schedules. This skill generates structured treatment plans following medical documentation standards, including patient assessment, diagnosis, treatment protocols, medication management, therapy recommendations, and outcome measurements, streamlining clinical documentation workflows while ensuring completeness.
What Is This?
Overview
Treatment Plans generates structured medical treatment plans for healthcare providers. It creates documentation covering patient assessment and history, diagnosis and clinical reasoning, treatment goals and objectives, intervention protocols, medication management plans, therapy recommendations, patient education topics, follow-up schedules, outcome measurements, and care team coordination.
The skill follows medical documentation standards including SOAP notes format, ICD coding references, evidence-based treatment protocols, and patient-centered goal setting. It generates plans appropriate for various specialties including primary care, mental health, physical therapy, and chronic disease management.
This standardizes treatment planning documentation ensuring nothing is missed while saving providers time on administrative work.
Who Should Use This
Primary care physicians creating comprehensive care plans. Mental health professionals documenting therapy plans. Physical therapists outlining rehabilitation protocols. Care coordinators managing chronic conditions. Any healthcare provider creating treatment documentation.
Why Use It?
Problems It Solves
Treatment plan documentation is time-consuming taking time from patient care. Automated generation produces complete plans in minutes.
Incomplete plans miss critical elements leading to poor outcomes. Structured generation ensures all necessary components are included.
Plans lack consistency across providers. Standardized formatting improves care team communication and handoffs.
Evidence-based protocols aren't always followed. Generated plans reference current clinical guidelines ensuring best practices.
Core Highlights
Structured treatment plan generation. SOAP notes formatting. ICD coding references. Evidence-based protocol recommendations. Medication management documentation. Therapy and intervention planning. Patient education components. Follow-up scheduling. Outcome measurement selection. Care team coordination.
How to Use It?
Basic Usage
Provide patient information, diagnosis, and treatment goals. The skill generates a comprehensive treatment plan.
Generate treatment plan for Type 2 diabetes patient with hypertensionCreate mental health treatment plan for anxiety and depressionDevelop physical therapy plan for post-ACL reconstructionSpecific Scenarios
For chronic disease management:
Create comprehensive care plan for COPD patientFor mental health:
Generate therapy treatment plan for PTSD using evidence-based approachesFor rehabilitation:
Develop post-stroke rehabilitation plan with functional goalsReal-World Examples
A primary care physician treats a newly diagnosed Type 2 diabetes patient. They generate a treatment plan including lifestyle modifications, metformin titration schedule, blood glucose monitoring protocols, diabetes education topics, referral to nutritionist, A1C monitoring schedule, and foot care instructions. The comprehensive plan ensures nothing is forgotten during the visit.
A physical therapist evaluates a patient after knee surgery. They generate a rehabilitation plan with specific ROM goals, progressive strengthening protocols, pain management strategies, home exercise program, functional milestones, and weekly visit schedule. The structured plan guides therapy sessions and measures progress objectively.
A psychiatrist treating depression creates a treatment plan including medication management with SSRI, CBT therapy sessions weekly, safety planning for suicidal ideation, depression screening scales for outcome measurement, lifestyle recommendations for exercise and sleep, and follow-up schedule. The comprehensive approach addresses all treatment dimensions.
Advanced Tips
Include measurable outcome goals for tracking progress. Reference specific evidence-based protocols when available. Document patient preferences and engagement in plan. Include barriers to treatment and mitigation strategies. Coordinate with multidisciplinary care team members. Update plans regularly based on response. Use patient-friendly language in education components. Consider social determinants of health.
When to Use It?
Use Cases
Creating comprehensive primary care treatment plans. Mental health therapy planning. Physical therapy and rehabilitation protocols. Chronic disease management. Post-hospitalization care planning. Preventive care protocols. Care coordination for complex patients.
Related Topics
Medical documentation standards. SOAP notes and clinical reasoning. Evidence-based medicine protocols. ICD and CPT coding. Patient-centered care planning. Chronic disease management models. Interdisciplinary care coordination.
Important Notes
Requirements
Patient clinical information and history. Confirmed diagnosis or assessment. Treatment goals and objectives. Understanding of relevant clinical protocols. Compliance with documentation standards. HIPAA and privacy compliance.
Usage Recommendations
Verify all clinical information accuracy. Customize generated plans to individual patient needs. Include patient in goal setting. Reference current clinical guidelines. Document patient education provided. Schedule appropriate follow-up. Measure outcomes systematically. Update plans based on response. Coordinate with care team members. Maintain privacy and security.
Limitations
Generated plans require clinical judgment and customization. Cannot replace clinical assessment and reasoning. Must verify medication dosing and interactions separately. Some specialties may require specific formats not covered. Cannot guarantee treatment outcomes. Requires provider review and approval. Must comply with institutional policies. Cannot include experimental or off-label treatments without explicit specification.
More Skills You Might Like
Explore similar skills to enhance your workflow
Brand Guidelines
Create comprehensive brand guidelines and style guides
Next.js Best Practices
Next.js conventions, RSC, data patterns, optimization
3D Web Experience
Build immersive, interactive 3D experiences and visualizations for the web
Viral Video Generator
Leverage advanced AI to generate high-engagement viral video content for social media platforms
Find Skills
Explore and integrate powerful new skills from the ecosystem to expand your AI assistant capabilities
Prompt Improver
Optimize prompts for better AI responses by transforming vague requests into clear and actionable instructions